Ultrasounds in physiotherapy apply to mechanical waves which spread out in the tissue. Because of the physical conditions, they are not visible. Everything which is not visible to the naked eye is easier to understand at a time when we deeply explore the essence of the phenomenon.
Physical Basics
The term “ultrasounds” applies to elastic waves with frequencies exceeding 16 kHz (sometimes the value of 20 kHz is assumed), which is above the upper limit of human hearing. The frequencies used in ultrasound therapy are typically between 800 kHz – 5 MHz. These waves must spread out in a particular medium such as air, liquid or solid (they cannot spread out in vacuum). Wave propagation velocity depends on the properties of the medium, in Chart 1 there are examples of physical data. The greater density and elasticity of the medium, the greater velocity. During the movement, the energy carried by the wave is suppressed due to a nonidealities medium. The physical measurement of this property is the absorption coefficient. To simplify, it can be assumed that fluids such as water or its solutions, and metals are good conductors of ultrasounds, while soft substances such as rubber, and silicone are bad ones. Soft tissues such as muscles and fat have indirect properties, due to the large amount of water in the cells. The energy carried by the wave in a medium with lossy properties is transformed into heat. The absorption coefficient dedicated for a particular substance depends on the frequency. The rule is that it grows with increasing frequency. Therefore, waves with lower frequencies allow for deeper medium penetration.
| Medium | Velocity [m/s] |
| Air | 331 |
| Water | 1493 |
| Aluminium | 6260 |
| Steel | 5900 |
| Hard rubber | 2300 |
Chart 1. Value of wave velocity in the selected mediums (based on “Ultradźwięki i ich zastosowanie” A. Sliwinski).
| Medium | Absorption coefficient | |
| 1MHz | 3MHz | |
| Water | 0,0006 | 0,0018 |
| Air | 2,76 | 8,28 |
| Blood | 0,03 | 0,09 |
| Adipose tissue | 0,14 | 0,42 |
| Nerve tissue | 0,20 | 0,60 |
| Muscles (longitudinal application) | 0,76 | 2,28 |
| Muscles (transversal application) | 0,28 | 0,84 |
| Blood vessels | 0,4 | 1,2 |
| Skin | 0,62 | 1,86 |
| Tendons | 1,12 | 3,36 |
| Caritilage | 1,16 | 3,48 |
| Bone | 3,22 | no data |
Chart 2. Based on: Medical rehabilitation 2000 volume 4 – special edition -„Jonoforeza i fonoforeza”
Another important phenomenon, which is of great practical importance, is the behaviour of the wave at the boundary of two mediums. If the properties of these mediums differ significantly, the wave is partially reflected. The remaining energy passes into another medium. In ultrasound therapy, we are dealing with relatively large wave energies introduced into the body. The power of ultrasound emitters is in the range of 2-30W, depending on the size and frequency of the head. Often we want to achieve the thermal effect, therefore, a matter of good wave transmission from the ultrasound head to the target tissue is very important. One of the medium parameters, which is used in the analysis of phenomena occurring at the boundary of mediums, is the acoustic impedance. In brief, we can say that the energy transmission is optimal (not reflected) if both mediums have the same impedance (similar to electrical systems). The greater the impedance difference, the greater the reflection. An example of such a medium arrangement is ultrasound head – air, where almost total reflection occurs. Due to the fact that the skin surface is porous in nature and often hairy to some extent, therefore it is difficult to avoid even a thin layer of air, which deteriorates the transmission. For this reason, the substances such as coupling gel or oil are applied. Another solution is to perform treatments in water, but in practice, this limits the application area to the limbs. Very often we have to deal with heterogeneous mediums in terms of structure, such as muscle or adipose tissue. In these cases, the medium contains a large amount of water which conducts the wave well, and a certain amount of harder structures and gases, which have small or similar sizes compared to the wavelength. In this case, the wavelength dispersion occurs.
| Transition | Reflection coefficient |
| ultrasound head – air | 0,999 |
| ultrasound head – coupling gel | 0,66 |
| coupling gel – skin | 0,001 |
| skin – adipose tissue | 0,009 |
| adipose tissue – muscles | 0,009 |
| muscles – bones | 0,34 |
| skin – air | 0,999 |
Chart 3. Reflection coefficient at the medium boundaries Based on: Medical rehabilitation 2000 volume 4 – „Jonoforeza i fonoforeza”
Cavitation
Cavitation is the phenomenon of generation and extension of pulsating gas bubbles in a liquid under the influence of the ultrasound wave with high intensity. This phenomenon is initiated above a certain level of intensity, known as the cavitation threshold. In brief, we can say that the acoustic wave causes a cyclic change of the local pressure in the medium. The greater the intensity of the wave, the greater the difference between the maximum and minimum pressure, wherein the pressure is always positive (there is no such thing as negative absolute pressure, it may be negative but in relation to some reference level). On the other hand, we know that the boiling point of a liquid decreases with pressure reduction. If the minimum value of the pressure associated with the wave activity will be lower than a certain threshold, then the local liquid evaporation process will be initiated. This produces a gas micro-bubble of saturated vapor of a particular liquid. In some situations, the bubble does not disappear in the phase of wave high pressure, but with subsequent cycles, it is getting bigger. This happens to a certain point when the process is losing stability and there is a sudden bubble “collapse” – implosion. Walls of the liquid molecules hit against each other at very high speed and power (on a micro-scale). Locally, enormous pressure is generated as is the temperature. This creates the conditions for the synthesis of chemical compounds which under “normal” circumstances do not exist. These phenomena are the subject of research and development of the field called sonochemistry.
In the case of ultrasound therapy, cavitation is a very harmful phenomenon and we should not allow for its development, because it causes the destruction of cellular and tissue structures. Therefore, the regulation concerning ultrasound equipment does not allow manufacturers to bring ultrasound heads to the market which emit waves exceeding 3W/cm2. However, studies indicate the formation of cavitation under certain conditions, even in the case of less intensity. Another unfavourable factor here is the heterogeneity of the emitted ultrasound wave.
Non-uniformity beam
Typical ultrasound heads used in ultrasound therapy are constructed with disks made of ceramic exhibiting piezoelectric properties. Under the influence of alternating voltage applied to the electrodes sputtered on the flat parts, the disk thickness is changed. Therefore, the front of the head can be treated as an approximation of the vibrating piston. Because the typical diameters of the transducers are greater than the length of the emitted wave, the beam has non-uniform intensity distribution. This phenomenon is caused by the interference of waves generated by individual fragments of the head. Particularly large heterogeneity is observed in the so-called near-field where treatments are usually carried out. In the far field, we observe a more uniform intensity distribution. For the ultrasound head, the 4cm2/1MHz field boundary is just 10cm from the front of the head. Figure 1 illustrates the characteristics of changes in the intensity of the wave on the transducer axis. Figure 2 shows the three-dimensional intensity distribution for the transducer with a diameter of 20mm, at a frequency of 2MHz and distances 6mm and 75mm from the head.
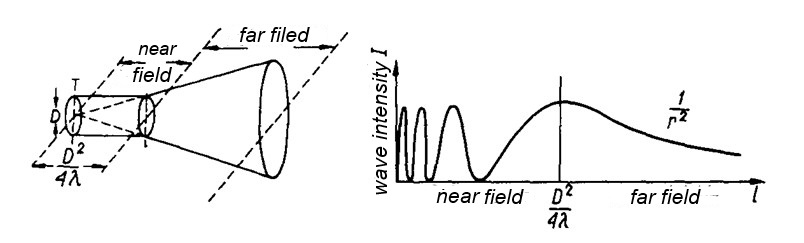
Figure 1. Wave intensity distribution on the circular transducer axis.
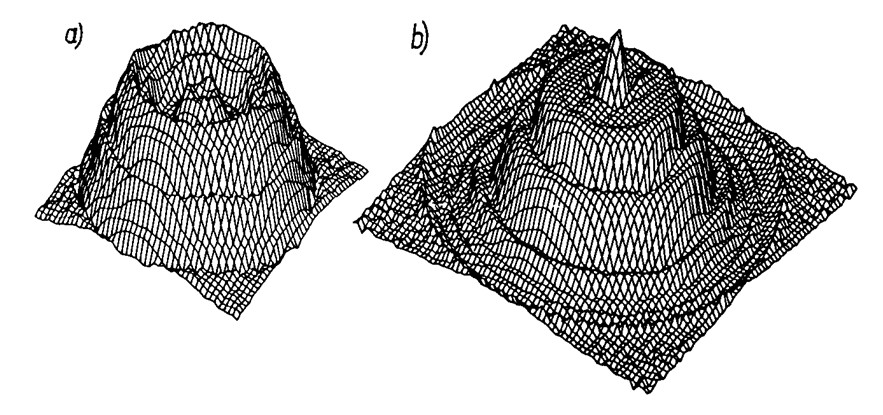
Figure 2 Three-dimensional intensity distribution at a distance of 6mm (a) and 75mm (b) from the head
Each ultrasound head should have a parameter, marked as BNR, which characterizes the heterogeneity of the emitted field. Usually, it falls within the limits of 5-8 and indicates how many times the maximum intensity (locally measured) is higher than the average intensity resulting from the quotient of power and radiation area. In practice, this means that if in the course of therapy, the set intensity is 1W/cm2 (typical, but not so big value), local therapeutic field intensity will vary from 0 to 6W/cm2 (for BNR = 6). Therefore, it is required to perform ultrasound head movements on the therapeutic area to avoid local overheating or even tissue cavitation. This is particularly important in the case of high doses, where the average intensity may exceed 2W/cm2. In such cases, it is recommended to apply pulsed mode, where the duty factor is 10-20 %, which significantly decreases the average power and we may avoid a strong thermal effect. An alternative might be conducting treatment in water in the far field.
Biological effects
Tissue heating is the most well-known and obvious consequence of ultrasound waves’ influence. As previously mentioned, the muscles and cartilage have a relatively large absorption coefficient, whereby ultrasound energy is converted into heat. This results in an increase in the pain threshold, muscle relaxation, and changes in nerve conduction. Tissue heating causes a secondary effect leading to an increase in kinetic energy, which results in increased enzyme activity within the ultrasound application area. Thus the metabolism is improved and regeneration processes are accelerated. Special attention should be paid to the larger absorption coefficient of cartilage and bones than muscles and adipose tissue. This can lead to a substantial increase in the temperature of these structures during treatment as well as exceed of therapeutic dose, and consequently damage to the tissue. The intensities above 2W/cm2 should be used very carefully, always perform ultrasound head movements and observe the patient’s feelings. If the patient experiences any specific pain around joints and bones, reduce the dose or use the pulse mode. The penetration depth can be controlled to some extent by the selection of the operating frequency of the ultrasound head. 1MHz ultrasound frequency results in deeper penetration than the frequency of 3MHz.
The ultrasound waves have also a purely mechanical impact associated with the generation of variable pressure within the therapeutic area. Tissues are subjected to a specific micro-massage occurring with the frequency of the ultrasound head. This leads to an increase in the permeability of cell membranes and the broadening of ion channels. In consequence, the metabolic processes occurring in cells are accelerated. Very important in this context is the ultrasound impact on the skin, particularly on the stratum corneum, which is the fundamental barrier that absorbs substances from the outside of the system. Mechanical wave impact results in a significant reduction of tightness of the stratum corneum and modulation of the size of sebaceous and sweat glands as well as hair follicles. Another factor increasing the permeability of the skin is the above-mentioned thermal effect. These phenomena have led to the development of transcutaneous drug application techniques.
Phonophoresis
Phonophoresis is a method of administering drugs through the skin by means of ultrasound influence. The active substance is dissolved in the gel, which is also the coupling medium between the skin and the ultrasound head. The main advantage of this method, as well as other transdermal ones, is to bypass the liver transition and concentrate therapeutic drugs in the treatment area. The limitation, in this case, is the relatively small amount of active substance due to the small thickness of the gel between the head and the skin. In addition, the drug particles penetrate into the skin only by diffusion forces, and they are also captured by the blood circulating in the vessels of the dermis. Therefore, phonophoresis therapeutic efficacy is limited to superficial diseases.
Electrophonophoresis
Electrophonophoresis is also a method of transcutaneous drug application but enhanced by the impact of electric current. The creator of this method is Dr A. Dyszkiewicz, who decided to combine both the advantages of iontophoresis (generation of a strong electric field gradient at the dissociated ions of the drug) and the influence of ultrasound waves (mainly modulation of the permeability of the skin and increase in the kinetic energy within the therapeutic area). For application, a special design of ultrasound head has been developed, which has a chamber for drug substances and an adequate current flow circuit. Because of the use of a direct current for the transportation of drug ions, the front of the head must have a layer with suitable chemical resistance to avoid chemical reactions with gel and then with particles of the drug. Conventional ultrasound heads frequently have heads made of aluminium alloy, which is a very reactive metal. For this reason, they are not suitable for such applications.
Because of the synergistic effects of ultrasound and ion transport in the electric field, electrophonophoresis method proved to be extremely effective when it comes to the treatment of topical diseases, located under the skin reaching even up to a few centimetres. It is especially valuable in the treatment of joint diseases, where the only alternative is standard pharmacotherapy or direct injection, both cases are subjected to side effects. Comparative studies conducted by Dr Dyszkiewicz on beef muscle cross-sections, using methylene blue dye showed a 4.5 – times greater penetration depth with the application of electrophonophoresis than phonophoresis. Compared to the standard ionophoresis, it penetrates 3 times deeper.
In conclusion, it should be noted that electrophonophoresis is a method of drug administration with high efficiency, and thus, it should be used with caution and under the supervision of a doctor. In the case of misdiagnosis or improper selection of the drug, the patient may suffer effects similar to wrong pharmacotherapy or injection.
The limitations of this method are the small knowledge about its application in medicine and the limited number of ready-made gels suitable for direct use.
